| Transmission Update:
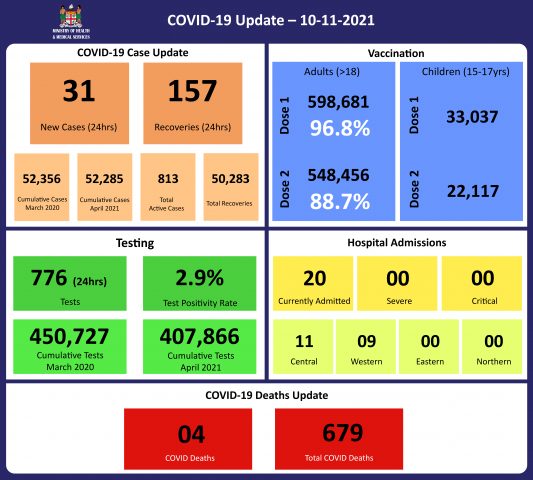
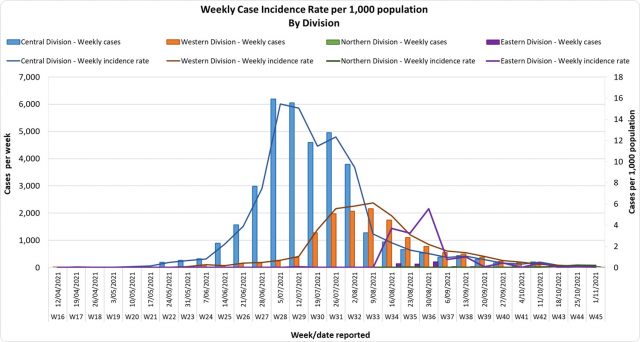
In the past 7 days, 55 cases were recorded in the central division, 29 new cases in the western division, 2 new cases in the eastern division, and 27 new cases in the northern division. The central division cases constitute 71% of the cumulative total cases nationally, with the western division making up 28% and 1% in the northern and eastern divisions. The 27 new cases recorded in the north are quarantine cases that are part of the repatriation program for the northern division. There is ongoing surveillance conducted for all repatriates. Since the last update, we have recorded 58 new cases of which 27 new cases were recorded on 09/11/2021 and 31 new cases in the last 24 hours ending at 8 am this morning. The national 7-day rolling average of cases as of 6th November is 16 daily cases. The weekly incidence rate graph by division indicates a continually declining trend. Furthermore, the peak weekly incidence in the western division was approximately a third of that in the central division, and the cumulative case numbers are also reflecting a similar difference. |
| Deaths:
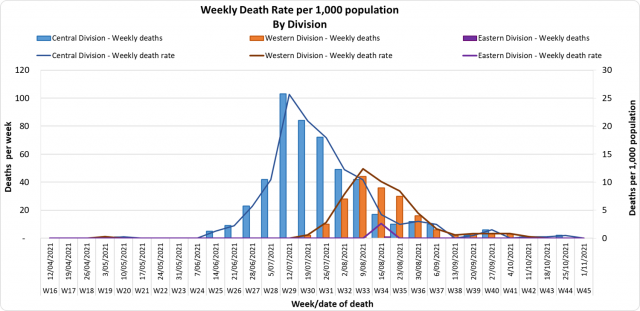
This curve depicts the weekly death rate per 1000 population by divisions since the 2nd wave of this outbreak began in April 2021. Overall the death rate graphs for the Central and Western Divisions indicate a declining trend. The differences between the Central and Western are similar to the incidence of the weekly cases and are likely a reflection of vaccination levels, COVID mitigation measures, and differences in population density. There are four COVID-19 deaths to report. The first COVID 19 death to report is of a 72-year-old man from the Western Division. He presented to the Sigatoka Hospital Emergency department in severe respiratory distress and died a few hours later on 16/10/2021. He was not vaccinated. The second COVID 19 death to report is of a 70-year-old man from the Western Division. He died at home on 01/09/2021 with severe respiratory distress and was not vaccinated. The third COVID 19 death to report is of a 75-year-old female from the Western Division. She died at home with severe respiratory distress on 06/08/2021. She was not vaccinated. The fourth COVID 19 death to report is of a 58-year-old male from the Western Division. He died at home with respiratory distress on 09/08/2021 and was not vaccinated. Kindly note that deaths from August and September are reported today because of a delay in the issuance of death certificates. There have been 679 deaths due to COVID-19 in Fiji, with 677 of these deaths during the outbreak that started in April this year. Please note that due to the time required by clinical teams to investigate, classify and report deaths, a 4-day interval is given to calculate the 7 days rolling average of deaths, based on the date of death, to help ensure the data collected is complete before the average is reported. Therefore, as of November 5th, the national 7 days rolling average of COVID-19 deaths per day is 0.1. The 7 days rolling average for COVID-19 deaths per day in the Central and Western Division 1s 0.0 and Eastern Division is 0.1, with a case fatality rate of 1.29%. We have recorded 578 COVID-19 positive patients who died from serious medical conditions they had before they contracted COVID-19; these are not classified as COVID-19 deaths. |
| Hospitalisation:
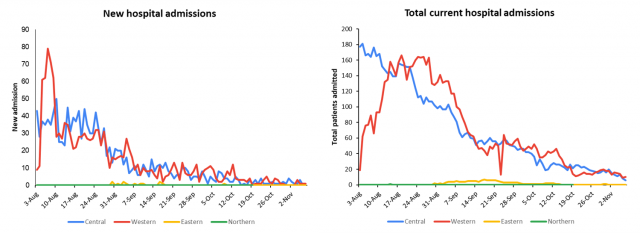
The downward trend in both the new hospital admissions and total admissions in all hospitals admitting COVID-19 patients across the country is consistent with the cases and death trends. The hospital admissions continue on a downward trend indicating a sustained positive response to COVID mitigation measures, Population density differences, and differential Vaccination rates. |
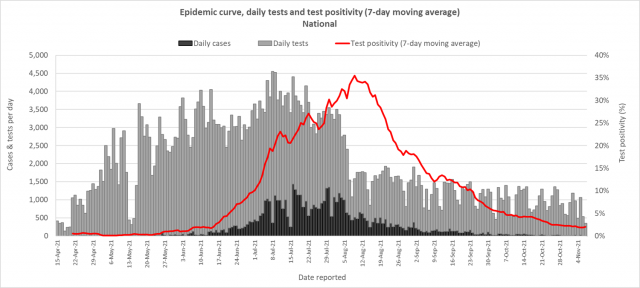
| Testing:
776 tests have been reported for November 9th, 2021. The 7-day daily test average is 745 tests per day or 0.9 tests per 1,000 population. The national 7-day average daily test positivity is 3.3%, which is below the WHO recommendation of 5%, and this is illustrated by the lab testing graph. Though we continue testing in high-risk areas, our case numbers and test positivity rate indicate a better control of the community transmission in Fiji through the combined efforts of containment and mitigation measures with ongoing community surveillance. |
Epidemic Outlook:
The Ministry of Health continues to monitor the outbreak using indicators such as daily case numbers, hospitalizations, test positivity, and deaths. There is a downward trend across all indicators of the COVID-19 epidemic in Fiji, indicating a positive response to our overall COVID containment and mitigation response.
With borders opening soon, we anticipate our testing numbers to increase from local and international repatriates as well as visitors entering the country.
Occupancy rates in health facilities, the occupancy rate of ICU beds, death rates, and vaccination coverage are indicators to monitor our health response capacity and we see a decreasing trend across indicators from our health facilities with increasing vaccination coverage for adults and 15-17-year-olds in Fiji.
Our weekly testing numbers of over 5,000 are still above the WHO recommended rate of 4 tests per 1,000 population per week (or approx. 3,500 tests per week) and we anticipate continued surveillance and testing in our communities and maritime islands to monitor and detect cases for early intervention.
Public Advisory:
A disease becomes endemic when it is expected to remain persistently present in the community. Some diseases endemic to Fiji are dengue fever and the common cold. These diseases persist at some level in the community and become epidemic when levels go beyond what is determined to be expected and acceptable.
Unfortunately, vaccine-related herd protection is not likely to be as efficient with COVID 19 as seen with some of the traditional vaccine-related diseases like measles. Those eligible must get vaccinated to reduce their risk of infection, severe disease, and death. And we know vaccines are very good in preventing severe disease and deaths.
This lower efficiency in vaccine-related herd immunity also means that the public will need to live with COVID safe measures of masking, hand washing, physical distancing, and good ventilation and/or air cleaning technology. These COVID safe measures remain vital in preventing the need to go back to severely restrictive public health measures.
Adjusting Our Quarantine Protocols
Our quarantine protocols to support international travel have been adjusted to take into account the increasing protection gained by having fully vaccinated persons traveling with other vaccinated persons to highly vaccinated destinations. This will involve less stringent conditions with more priority given to the testing protocols that ensure early identification and isolation of positive travelers. From the 11th of November, we will be transitioning Border Quarantine Protocols to Border Risk Reduction Protocol for all travelers coming in from Travel Partner Countries This will involve a 3 day stay in a hotel with a test to be done on day 2. A negative result will allow for discharge into the community on day 3.
From the 11th of November incoming travel will be restricted to diplomates, returning residents, permit holders, and those approved by the Covid 19 Risk Mitigation Taskforce. Our Border Risk Reduction Protocol Processes will be trailed during this time and further refined in preparation for the 1st of December. Approvals to home quarantine will be extremely limited during this pilot phase.
Changes to domestic travel quarantine protocols will be announced tomorrow once vaccination coverage data in Vanua Levu and some of the maritime islands is obtained. The MHMS have escalated preparedness and response plans to mitigate against and manage surges in cases though:
- Early warning system set up in all maritime islands and oversight in place to ensure 100% weekly reporting of Acute respiratory illness and Febrile illness from all facilities
- Prepositioning of Air, Land, and Sea-based capability to facilitate retrieval of cases within Vanua Levu and from Maritime Islands to sub-divisional and divisional hospitals
- The clinical capability has been escalated in health centers and nursing stations to facilitate early diagnosis, monitoring, and referral of sentinel cases.
- Testing capacity has been escalated in Viti Levu to support travel to the North and Maritime islands
- Clinical Care capability in the 3 divisional hospitals have been escalated
- Reviewing and strengthening clinical care protocols for severe disease in all sub-divisional and divisional hospitals
Supporting School Re-opening
COVID-19 poses a lower risk to children however secondary transmission from young school-age children can and does occur in both household and school settings. With good vaccination coverage, high levels of COVID safe adherence, and timely instigation of measure as done in this case, it is possible for us to facilitate a measured containment program whilst continuing the school program whenever we find a positive student in school. This case and similar cases, even if truly positive, will help to refine the implementation of COVID safe measures in schools and help to put in place a quality improvement framework around the program to promote the safe opening of schools.
Students are reminded again of the need to maintain proper masking practices at all times, remain as much as possible in open ventilated spaces when with their friends, and follow all COVID safe measures especially when indoors.