COVID-19 Situation Update
Wednesday 26th January 2022
| Transmission Update:
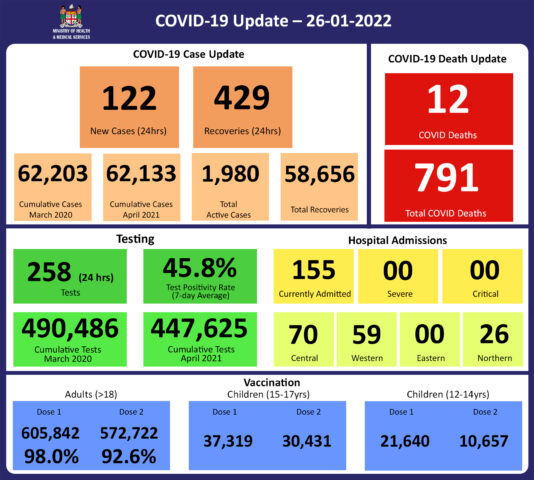
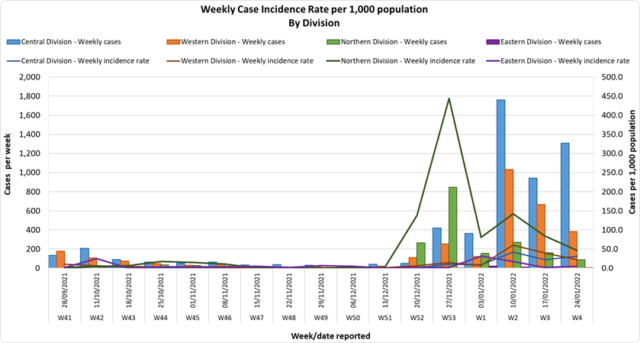
In the past 7 days until 25/01/2022, 1,162 new cases were recorded in the Central division, 210 new cases in the Western division, 1 new case in the Eastern Division, and 51 new cases in the Northern Division. The Central Division cases constitute 68% of the cumulative total cases nationally, with the Western division making up 28%, 3% in the Northern Division, and 1% in the Eastern Division. Since the last update, we have recorded 223 new cases of which 113 new cases were recorded on 25/01/2022 and 110 new cases in the last 24 hours ending at 8 am this morning. Of the 223 cases recorded, 116 cases were recorded in the Central Division; 92 cases were recorded in the Western Division, 11 cases were recorded in the Northern Division, and 4 cases were recorded in the Eastern Division. The national 7-day rolling average of cases as of 22nd January is 246 daily cases. |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Deaths:
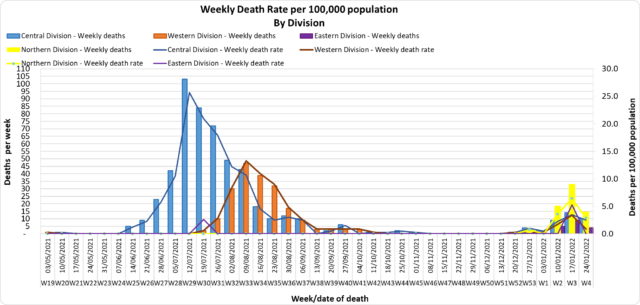
This curve depicts the weekly death rate by division since May 2021. Overall, as of the week of 17/01/2022, the death rate graph indicates an upward trend in the number of COVID-19 deaths in the Central, Western, Eastern, and Northern divisions. Please note the week of 24/01/22 (this week) is not yet complete therefore the appearance of a downward trend may not be accurate. There are also deaths in the Western Division currently under investigation for the same time period, therefore the rate for that division may increase. Analysis of deaths in the third wave Table 1: Death rates by Division
An analysis of the first 94 deaths recorded in the third wave has shown that, while the Central Division has the highest absolute number of deaths, the Northern Division has the highest rate of death when adjusted for population. Note that there are deaths currently being investigated from the Western Division for the same time period, therefore the rate for that division may increase. Table 2: Deaths by age group
For the first 94 deaths in the third wave, the rates of death, when adjusted for population, have been highest in the age groups beginning from age 50 and upwards. The 5 deaths in the under 19 group were for children with significant underlying medical conditions present since birth. Table 3: Deaths by Vaccination Status
An analysis was done for the first 91 deaths in the vaccine eligible population during the third wave. When adjusted for population in the fully vaccinated (received 2 doses) and unvaccinated (received 0 doses) adults in Fiji, we can see that death rates per 100,000 population are 6.1 deaths per 100,000 for fully vaccinated adults and 90.2 deaths per 100,000 for unvaccinated adults. This means that unvaccinated adults in Fiji have been dying from COVID-19 at a rate 14.7 times higher than fully vaccinated adults during this third wave. The 2 individuals in the 12-17 age group who died were not vaccinated. There have been no deaths in individuals who have received a booster dose (3rd dose) of the vaccine. New deaths to report There are 12 new COVID-19 deaths to report from the period 8th January 2022 to 22nd January 2022. Two deaths were from the Central Division, five from the Western, one from the Eastern, and four from the Northern. Three of the individuals who died were below the age of 18 years old and were not eligible for vaccination. Two individuals had congenital medical comorbidities from birth, which contributed to the severity of their sickness and demise. Out of the nine individuals who were in the target age group for vaccination, six people were fully vaccinated and three were unvaccinated. The deaths of individuals below the age of 18 were reported today after a thorough investigation done by the Ministry. The first COVID-19 death to report is of an 8-year-old female from the Northern Division. She died at home on 12/02/22. She had a significant congenital medical condition that likely contributed to her death. She was not eligible for vaccination. The second COVID-19 death to report is of a 13-year-old male from the Northern Division. The child presented to Nabouwalu Hospital on 06/01/2022 and was admitted. Sadly, he died on 15/01/2022, nine days after his admission. He had a significant congenital medical condition, and an assessment made by medical consultants confirmed that his pre-existing conditions contributed to his death. He was not vaccinated. The third COVID-19 death to report is of a 70-year-old male from the Northern Division, who died at home on 14/01/2022. He was not vaccinated. The fourth COVID-19 death to report is of a 10-day old female infant from the Northern Division. The infant was born to a COVID-positive mother, without any complications at birth. She sadly passed away at home before she could be brought to the hospital. A post-mortem COVID test was noted to be positive. She was not eligible for vaccination. The fifth COVID-19 death to report is of a 98-year-old female from the Western Division, who died on arrival at Lautoka Hospital on 16/01/2022. She was fully vaccinated. The sixth COVID-19 death to report is of an 81-year-old female from the Western Division, who died at home on 16/01/2022. She was fully vaccinated. The seventh COVID-19 death to report is of a 74-year-old male from the Western Division, who died on arrival at Tavua Hospital on 18/01/2022. He had pre-existing medical conditions and was not vaccinated. The eighth COVID-19 death to report is of a 75-year-old female from the Western Division, who died at home on 20/01/2022. She was fully vaccinated. The ninth COVID-19 death to report is of a 72-year-old female from the Central Division, who died at home on 21/01/2022. She had pre-existing medical conditions and was fully vaccinated. The tenth COVID-19 death to report is of a 46-year-old female from the Western Division, who died at home. She was not vaccinated. The eleventh COVID-19 death to report is of a 78-year-old male from the Eastern Division, who died at home on 21/01/2022. He was fully vaccinated. The twelfth COVID-19 death to report is of a 79-year-old male from the Central Division, who died on arrival at CWM Hospital on 22/01/2022. He was fully vaccinated. There has been a total of 791 deaths due to COVID-19 in Fiji. Please note that due to the time required by clinical teams to investigate, classify and report deaths, a 4-day interval is given to calculate the 7 days rolling average of deaths, based on the date of death, to help ensure the data collected is complete before the average is reported. Therefore, as of January 20th, 2022, the national 7 days rolling average for COVID-19 deaths per day is 4.1, with a case fatality rate of 1.32%. We have recorded 774 COVID-19 positive patients who died from other serious medical conditions unrelated to COVID-19; their doctors determined that COVID-19 did not contribute to their deaths, therefore these are not classified as COVID-19 deaths. |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Hospitalization:
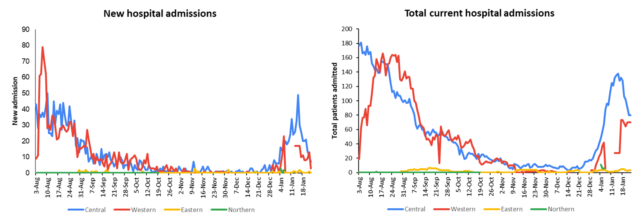
There is a downward trend in daily hospitalisations. Using the WHO clinical severity classification, a greater percentage, 54% (n=84) of the admissions of COVID-19 positive patients are categorized as asymptomatic and mild, 24% (n=37) are categorized as moderate and 19% (n=29) as severe with 5 cases in the critical category. Anyone admitted to the hospital is tested before admission, therefore, a significant number of people are admitted to the hospital for non-covid health conditions, but incidentally, test positive due to the high amount of transmission in the community. The number of people being admitted because of COVID-19 remains low. |
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Testing:
258 tests have been reported for January 25th, 2022. The 7-day daily test average is 458 tests per day or 0.5 tests per 1,000 population. The national 7-day average daily test positivity is 45.8%. The high positivity rate is an indication of widespread community transmission. |
Public Advisory:
The analysis of the first 91 deaths in the vaccine eligible population during this third wave has revealed that fully vaccinated adults have an almost 15 times lower rate of death from COVID-19 than unvaccinated adults. This is comparable to rates seen overseas, which is an indication of the quality of our COVID-19 vaccination program, even with the urgency of ensuring rapid deployment of vaccines in a very short time period. A testament to the work put in by our dedicated health teams and partner agencies to ensure that protocols are followed, and vaccines are administered properly to the people of Fiji. The huge difference in death rates between vaccinated and unvaccinated adults is even further evidence that vaccines work to prevent severe outcomes of COVID-19.
We also continue to record lower than expected hospitalizations due to COVID-19 despite the current resurgence in COVID-19 cases throughout Fiji. This decoupling of the relationship between cases and severe outcomes is a result of the protection afforded by the vaccination program. The reported deaths today (including the three children) have been confined to individuals with high medical risk and who have died, either at home, on the way to the hospital, or within a few days of admission. These 2 factors (comorbidity and adverse health-seeking behavior) also make it difficult to narrate more precisely the extent to which COVID 19 contributes to the death of patients.
The deaths of the 3 children announced today are a sad reminder of the legacy of COVID 19; that, as cases increase to very high numbers in the community, our most vulnerable are at increased risk of being infected and suffering from severe disease. We know that severe disease is rare in children, but this risk increases should they have significant underlying health conditions.
By vaccinating and maintaining our COVID safe measures, we protect the vulnerable among us. We have mentioned in the past that the vaccines are 80% protective against severe disease and death and not 100%. As such, if community transmission is high enough, rare outcomes will become more frequent.
Looking after the vulnerable needs to be a community-wide effort. The public needs to be aware of the symptoms of severe COVID-19 disease, and early presentation to a health facility when severe symptoms are present, are critical protection measures that we should know and act upon.
The severe symptoms to look out for are: having trouble breathing (shortness of breath or difficulty breathing), ongoing chest pain, severe headache, confusion, inability to stay awake or wake up, pale, grey or blue-colored skin, lips or fingernails, worsening weakness, coughing blood.
Non-communicable diseases (NCDs) and COVID-19
Based on severe disease and death data, it is obvious that nationwide resilience building will need to focus on preventing our developing chronic diseases, and ensuring that those with chronic diseases are well controlled. Both involve building up the good habits of exercise and a healthy diet, and good attendance to medical follow-up and ongoing treatment for those with chronic disease.
Our health statistics over the last few years show that over 80% of total deaths in Fiji are attributed to NCD deaths, and between 30-40% of these are premature deaths. To put an average figure on NCD deaths per year, we record around 5828 deaths annually (average 2015-2020). NCDs have been on the rise for many decades, and whilst this is partly due to better reporting, the inescapable fact is that lifestyle changes need to be made at a community-wide and individual level. The 3 waves of COVID 19 have clearly demonstrated the need for each of us to choose healthier lifestyles and to support each other when one makes such a choice. Choices around physical activity, food portions, and food choices are now more important than ever before. This virus and its many variants will remain endemic for a long time to come and the consequences will reduce BUT OVER A LENGTH OF TIME.
Even if you have a chronic disease, making the healthier choices outlined above will make you stronger and more resilient in the face of this virus.
Employers and community leaders can help to mainstream the support system for vulnerable persons by creating a list of vulnerable persons in their communities, providing support to help them secure good access to medical care, ensuring oversight so that the vulnerable are tested early when they develop flu-like symptoms and provide a supportive environment to ensure that the sick are encouraged and empowered to seek treatment and not delay in seeking health care. In this way, we are working together to protect the most vulnerable, and to direct health care service towards those who need it most in our community.
Promotion of Better Health Seeking Behavior
The Ministry will continue to strongly promote better health-seeking behavior moving forward. The Ministry had committed to facilitating regular outreach services and undertaking community-wide health awareness and promotion activities even before this pandemic. We have escalated our effort further during the current pandemic, however, it is clearly visible from the death data that untimely seeking and accessing health care remains a crucial challenge. The Ministry recognizes that there are factors outside the health sphere that impact health-seeking behaviour, and we appeal to everyone to assist in addressing these factors so that the impact and benefits of health care are appreciated by all who need the care.
Vaccination
The booster dose program began at the end of November 2021. As of January 24th, 68,099 individuals have so far received booster doses of the Moderna COVID-19 vaccine from the 142, 240 persons considered eligible. This represents a 48% coverage rate for booster-eligible persons. We are also expecting to receive more Pfizer vaccines soon which will be used for booster doses and as a vaccine for children. The booster vaccine and vaccination for children are not considered mandatory, however, we encourage all eligible individuals to be vaccinated or get a booster dose, and help navigate Fiji into a safer covid zone that supports the socio-economic revival and safer reopening of schools.
Vaccination of children under 12 years remains part of ongoing discussions as sourcing them remains difficult.
International Travel
International travel will continue to need ongoing reviews. We note the WHO advice that national authorities should lift or ease international traffic bans, as they do not provide added value, and continue to contribute to the economic and social stress in countries. In addition, they can adversely impact global health efforts during a pandemic by disincentivizing countries to report and share epidemiological and sequencing data.
We will however continue to apply a multi-layered risk mitigation approach to potentially delay the exportation or importation of the new variant, including via the use of entry/exit screening, testing, or quarantine of travelers. These measures should be informed by a risk assessment process and be commensurate with the risk, time-limited, and applied with respect to travelers’ dignity, comfort, convenience, and rights.
We will continue to ensure adequate measures such that all travelers are screened for signs and symptoms of COVID-19, are vaccinated, and adhere to public health and social measures at all times
Building Resilience
As we go through the current wave of COVID-19, Fijians need to adopt practices that build resilience. We know that there remains a high risk of resurgence of endemic variants and the arrival of new variants. Our socioeconomic survival depends on our ability to build and sustain individual and community-wide resilience. We should expect that COVID-19 will be endemic, however, we need to appreciate that “endemic” doesn’t mean harmless. Endemic means that we expect continued circulation of the disease in the community, the baseline levels of which are yet to be determined. Leptospirosis, Typhoid, and Dengue are endemic in Fiji and they are associated with serious outcomes, especially when the number of cases increases to outbreak levels. Building resilience means that we must adopt healthier lifestyles, make COVID safe behavior a habit that we adopt and support others to adopt, mainstream medical and community-wide oversight over vulnerable persons so they can have timely access to health care, and build up community surveillance mechanisms that use health and non-health data sources to alert us of impending disease outbreaks.
Our objective is to live with the virus and at the same time ensure a high level of transmission suppression, and prevention of severe outcomes.